Vascularised lymph node transfer (VLNT)
The key facts
|
|
|
|
|
About the treatment
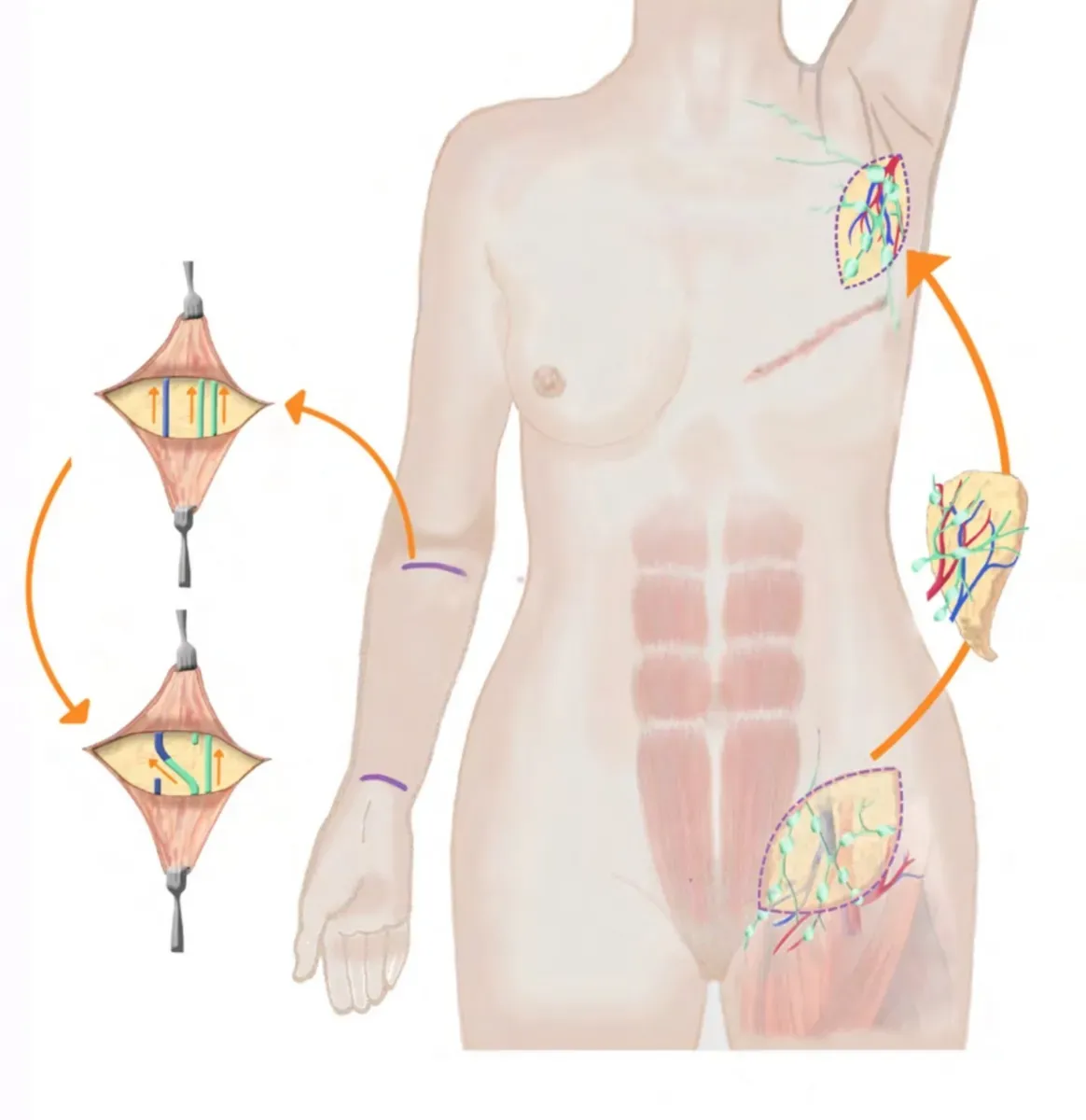
In vascularised lymph node transfer, a small section of tissue containing lymph nodes – usually with a small patch of skin for better monitoring – is removed from another region of the body and transplanted into the region affected by lymphoedema. The tissue is transplanted together with the associated blood vessels (revascularised) so that it remains supplied with blood and functional.
Possible donor sites include the groin, neck area or abdomen. It is particularly important that the donor site is carefully selected so as not to cause any new lymphatic drainage problems there.
Receptor vessels are blood vessels that are not crucial for blood circulation to the extremities. This allows the transplanted lymph node tissue to create new drainage pathways for the accumulated lymph fluid, improving the symptoms of lymphoedema in the long term.
In some cases, lymph node transfer can also be combined with the LVA method – either in the same operation or at a later stage. We will discuss with you whether this procedure is suitable for you during our specialist lymphatic surgery consultation.
Typical areas of application
- Chronic lymphoedema following cancer treatment (e.g. breast, abdominal or skin cancer)
- Secondary lymphoedema following lymph node removal or radiotherapy
- Advanced lymphoedema with persistent symptoms despite conservative treatment
- Recurrent infections (e.g. erysipelas) caused by impaired lymph drainage
- Restricted mobility or function due to chronic swelling
- Insufficient success with LVA (lymphaticovenous anastomosis) alone
When is it recommended?
- When non-surgical measures have been exhausted (compression, lymphatic drainage)
- When the lymphoedema is stable enough for a microsurgical procedure
- If the patient is prepared to undergo lifelong aftercare (e.g. compression therapy)
- In the case of localised swelling that can be treated surgically in a targeted manner
- When the aim is to achieve long-term improvement in symptoms and better quality of life
- In combination with LVA, if both methods can complement each other effectively
“Lymphoedema is restrictive not only the body, but also on a patient’s life. With innovative lymphatic surgery, we can help to significantly reduce this burden."
FAQs
Where are the lymph nodes removed from – and is there a risk of developing new lymphoedema in that area?
The lymph nodes are removed from areas such as the groin or abdomen. In doing so, we take great care to select only areas where the risk of new lymphoedema is minimal.
How long does it take to heal after the operation?
The wound takes approximately 2 to 4 weeks to heal. Many patients notice initial improvements in lymphoedema after a few months, as the lymphatic system slowly reorganises itself.
Will the swelling be gone permanently?
The aim of the procedure is to achieve a long-term reduction in swelling and improve quality of life. Complete regression cannot be guaranteed, but many patients benefit significantly.
Booking options


